September is Polycystic Ovarian Syndrome Awareness Month. We are continuing our series about the diagnosis and treatment of this commonly occurring disease in reproductive-age women.
In Part I, it was determined that polycystic ovarian syndrome, commonly referred to as PCOS, is the most common hormonal disorder affecting women of reproductive age throughout the United States. This is why it is so important that PCOS be diagnosed as early as possible. However, diagnosing PCOS can sometimes be difficult, as there is no specific test for the disease and patients can present with a wide variety of symptoms. Generally, patients with irregular periods who also exhibit signs of androgen excess in the form of surplus excess hair growth and acne (as described in Part I last month) are considered to have PCOS – insomuch as other medical conditions have already been excluded.
Approved Diagnostic Measures: How Reproductive Endocrinologists Identify PCOS
In order for a diagnosis of PCOS to be made, a patient must present with at least two of three criteria that include irregular menstrual periods; signs of androgen excess, such as excess hair growth; and typical appearance of polycystic ovaries revealed by an ultrasound. Currently, PCOS in women is diagnosed using three primary measures:
• Physical Exam – During a complete physical exam, the physician examines the patient for telltale signs of androgen excess. The skin manifestations of PCOS include acne and excess facial hair growth on the sideburns, upper lip and chin. Because patients with PCOS also have a higher incidence of heart disease and diabetes, it is important for blood pressure, height, weight and abdominal girth to be measured.
• Lab Tests – Before a patient can be diagnosed with PCOS, other hormonal disorders must be ruled out using lab tests. Some of the disorders to rule out include thyroid disease, hyperprolactinemia, Cushing’s syndrome and congenital adrenal hyperplasia. Blood tests such as luteinizing hormone (LH), follicle stimulating hormone (FSH), testosterone and dehydroepiandrosterone sulfate (DHEAS) can also help confirm the diagnosis of PCOS. Because PCOS patients are at risk for diabetes and high cholesterol, additional tests may be performed. Traditionally, the glucose tolerance test (GTT) is used, and involves the patient drinking a sugary solution. Blood tests are drawn before the patient consumes the solution and then again two and three hours afterward. For this test, it is important not to eat or drink for 12 hours prior. Cholesterol levels including high-density lipoproteins (HDL), low-density lipoproteins (LDL) and triglycerides can also be measured.
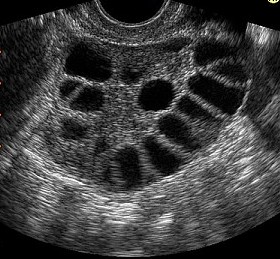
• Pelvic Ultrasound – A pelvic ultrasound may be performed to look for follicles in the ovaries. Typically, at least 12 small follicles are seen in each ovary measuring two to nine millimeters in diameter. It is important to note that many women with PCOS have ovaries that appear normal by ultrasound.
Polycystic ovarian syndrome is a common hormonal disorder that impacts women throughout the United States. It is important for women of reproductive age, who plan to conceive or have experienced difficulty conceiving, to consult with a physician to determine if PCOS is inhibiting fertility. Diagnosing PCOS is the first step toward ensuring that fertility is optimized and receiving the necessary treatment.